Mitochondrial Stem Cell Research
Main content
Human pluripotent stem cells (iPSCs) offer a unique opportunity to model human disease in a renewable and tissue-specific manner. IPSC can also be used in large-scale screening of potential therapeutic agents. Further, using new technology that allows us to correct the genetic defect in living cells, iPSC provides a potential form of treatment themselves.
The MMN group, previously led by Prof. Laurence Bindoff, is also part of Neuro-SysMed, a Center of Excellence for Clinical Research in Neurological Diseases at the Department of Neurology, Haukeland University Hospital. Currently, the mitochondrial stem cell research group is led by senior researcher Dr. Kristina Xiao Liang as the group leader and principal investigator. This work was done in close collaboration with Gareth Sullivan at the University of Oslo.
We are using stem-cells transformed from the patient’s own fibroblasts to study the mitochondrial disease caused by POLG mutations. These “induced pluripotent stem cells” (iPSC) offer a unique opportunity to model human disease in a renewable and tissue-specific manner. Thus far we have successfully generated neurones and all glial cell types, cardiomyocytes, and hepatocytes from these iPSCs.

Aims
The group’s current research aims are to perform in vitro iPSC-based model system research to increase the knowledge in POLG diseases and to identify the mechanisms underlying this common type of mitochondrial disease. From this work, we will develop an iPSC-based platform to test the therapeutic agents.
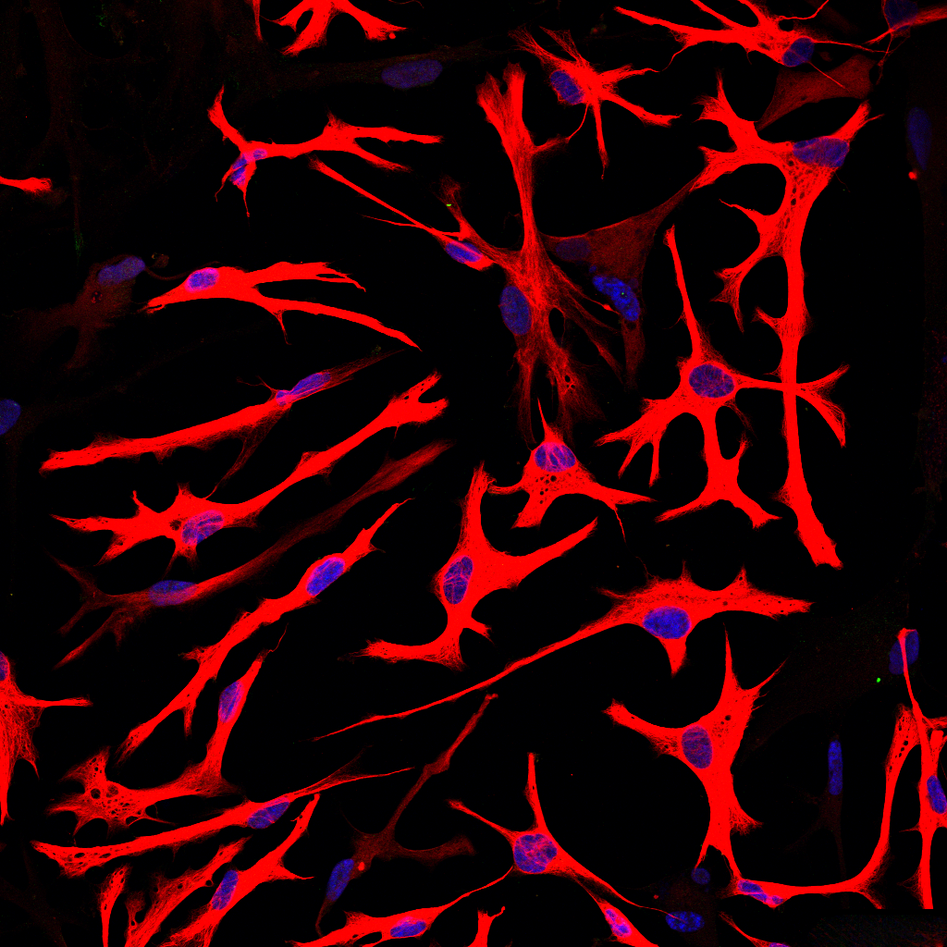
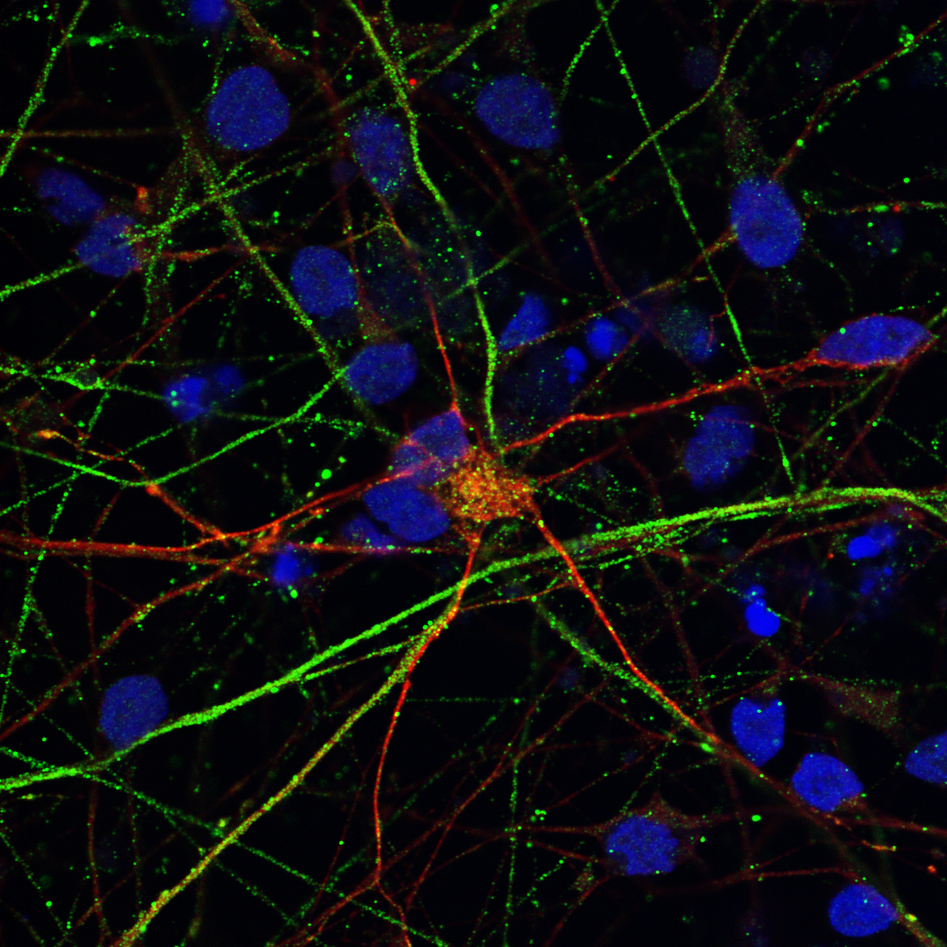
We have established the required competence and facilities for human induced pluripotent stem cell (hiPSC) reprogramming and differentiation, enabling investigation of neuronal cells from patients and healthy controls. Validated iPSCs are differentiated to neural stem cells (NSCs) and regionalized neuronal subtypes, as well as astrocytes/ glial populations. A postdoctoral fellow in our group, Yu Hong, has developed brain organoids and will be using these both to investigate disease mechanisms and to test treatments.
Our efforts to identify the biological and pathological basis of the neurodegenerative disorder associated with mitochondrial dysfunction have resulted in several translational publications and we aim to develop this and perform more deep molecular phenotyping studies. As this group is also part of the Neuro-SysMed center, we will use our models and stem cell approaches to study other neurodegenerative diseases such as Parkinson's disease and Alzheimer's disease.
Projects
Multiple iPSC-based in vitro model systems.
- 2D: neural stem cells, DA neurons, motor neurons, generic neurons, astrocytes, oligodendrocytes and cardiomyocytes.
- 3D: mini-brain organoid system
- Co-culture systems
Modeling diseases using neural stem cells, neurons, astrocytes, and astrocyte-neurons interactions.
Developing a high-throughput iPSC-based platform for screening the therapeutic agents.
Investigating metabolic reprogramming between the neurons and glial cells
Using single-cell transcriptomics for multidimensional phenotyping.
Cooperation
We are part of the Neuro-SysMed, Center of Excellence for Clinical Research in Neurological Diseases. Our group is also one of the founder members of the Bergen Stem Cell Consortium (BSCC). The BSCC received strategic funding from the Regional Health Authority and is in the process of establishing new laboratories, including a GMP facility, in the hospital. It comprises groups working with different types of disease from cancer to diabetes
Additional collaborative interactions include:
- Department of Neurology, Division of Basic Neuroscience Research. Harvard University, USA.
- Institute of Basic Medical Sciences, University of Oslo, Norway.
- Faculty of Medicine, University of Oslo, Norway.
- The Norwegian Center for Stem Cell Research, Oslo University Hospital-National Hospital, Norway.
- Department of Biomedicine, University of Bergen, Norway.
Funds
- NFR
- UiB
- Helse Vest