Research activities and highlights
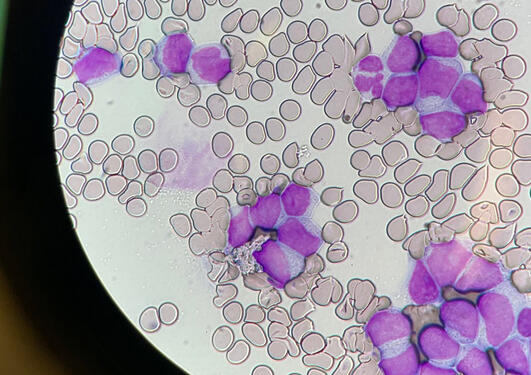
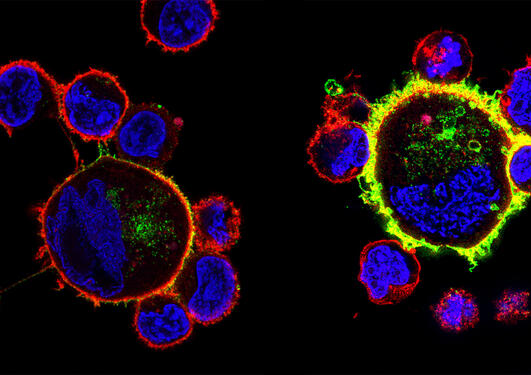
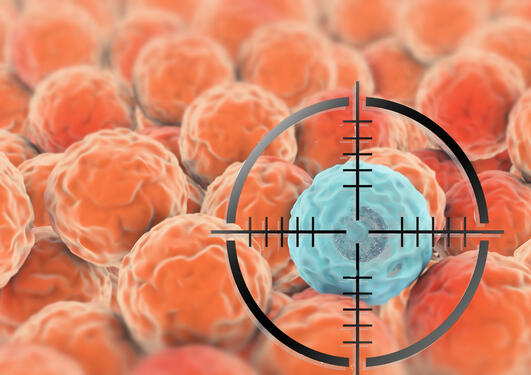
CCBIO has a focus on tumor-microenvironment interactions and plasticity programs in primary and metastatic lesions and how these can define aggressive tumor phenotypes and predict cancer progression and treatment response. CCBIO has three overlapping and well integrated research areas: basic studies of cancer mechanisms, discovery and validation of cancer biomarkers, and clinical studies.

Main content
An ambition is to obtain rapid transfer of knowledge to practical medicine. Since the opening of CCBIO in 2013, several research projects have been initiated and are now (2016) running in different teams, with increased internal collaboration and external networking.
Below you can find research progress in each group for the last two years, and a comprised overview of highlights from the first four years.