Meet our recent doctoral graduates
Congratulations to BCEPS PhD candidates Lelisa Fekadu and Getachew Teshome on successfully defending their doctoral theses this spring.

Main content
Both Lelisa and Getachew have been part of Disease Control Priorities - Ethiopia (DCP-E), a project funded by the Bill and Melinda Gates Foundation (BMGF). They were selected following a national, open competition by Ethiopia's Federal Ministry of Health (FMOH), BCEPS Director Ole Frithjof Norheim and Stéphane Verguet at Harvard T.H. Chan School of Public Health (HSPH).
Norheim comments as follows:
Lelisa Fakadu and Getachew Teshome have really impressed me with their dedication and hard work. By completing their PhDs in such a good way, DCP-Ethiopia has also delivered on one of the two promises we gave to the Ministry of Health and the Gates foundation: to strengthen country capacity in health economics and priority setting. I believe they will lead the way for fair and efficient priority setting in the Ethiopian health system.
Revising Ethiopia's Essential Health Service Package
In 2005, Ethiopia's FMOH established a national Essential Health Services Package (EHSP). The original intention was to revise the package every 5 years. However, a lack of evidence and technical capacity meant that such regular revisions were not possible. With EHSP no longer meeting the key national policy goals, DCP-E's objective has been to increase Ethiopian researchers' and policy makers' competence to enable a revision of the package. As part of their doctoral programme, the PhD candidates were trained in health economics, decision sciences and priority setting. Learning about the latest knowledge and methods in evidence-based, cost-effective health priority setting approaches allowed them to gather and evaluate evidence needed to update FMOH policies.
Research contributions
Utilising their new skills, Lelisa and Getachew generated an evidence base for designing, developing and implementing essential health services in Ethiopia. Both doctoral theses consist of three individual papers, each with a specific objective contributing to a general goal.
The aim of Getachew Teshome's thesis was to review the current EHSP in Ethiopia and provide input to the design of a revised primary health care package with the following sub-objectives:
- To estimate the national and subnational Universal Health Coverage (UHC) status of Ethiopia in the year 2015
- To generate cost-effectivness evidence for relevant health interventions using the World Health Organization's generalised cost-effectiveness approach
- To describe the revision process, stakeholders' and experts' involvment and the most important features of the new Ethiopian EHSP
The most relevant findings include establishing that the baseline (2015) UHC service coverage index for Ethiopia was low. There is vast sub-national variation, as well as between programme areas. Furthermore, several potential cost-effective interventions were available that could substantially reduce Ethiopia’s disease burden if scaled up.
Lelisa Fekadu's thesis focuses on Ethiopian health interventions for three specific diseases with high burden and economic impact, namely HIV, Tuberculosis and Malaria. The general objective of his doctoral thesis was to provide evidence on the patient cost, health gains and financial risk protection of HIV, TB and malaria interventions across socio-economic groups in Ethiopia.
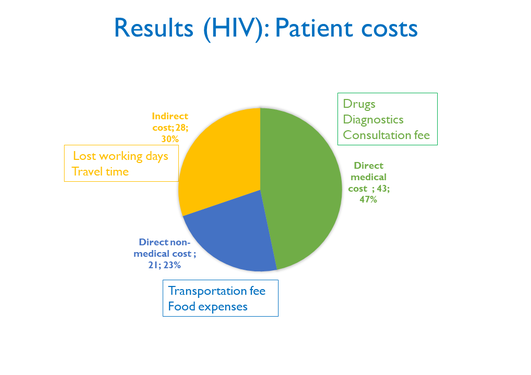
- To estimate direct costs, indirect costs, catastrophic health expenditures, and its determinants across socioeconomic groups for household affected by HIV and TB
- To assess the expected health gains and financial protection benefits from the public financing of selected malaria prevention and treatment interventions across socioeconomic groups
- To assess the expected health gains and financial protection benefits from the public financing of selected TB interventions across socioeconomic groups
Lelisa found that HIV and TB treatment put a huge financial burden on households, which disproportionately affects those in the lowest socio-economic group and results in catastrophic expenses. The study also suggests that Ethiopia's current policy of exemption from payment for health services is insufficient to cover all necessary patient costs and protect people from financial difficulties. Based on his findings, Lelisa recommends Ethiopian authorities to implement patient-centered care and expand publicly funded health services to better protect against poverty and reduce the financial burden on vulnerable households.
Future plans
Both Lelisa and Getachew have expressed a wish to continue contributing to the implementation of fair and efficient priority setting processes in the Ethiopian health system.