Research areas
Medical ultrasound is an imaging technique with both diagnostic and therapeutic applications. Methods and research areas include:
Main content
Three-dimensional ultrasonography
Three-dimensional ultrasonography (3D) is developed for various organ systems, allowing both volume determination and visualization. The 3D ultrasonography systems are sophisticated, producing highly accurate and precise volume estimates with low intra and inter observer bias. Volume and surface rendering enable 3D reconstructions of organs helpful in asserting functionality and segmentations of liver tumours among other applications.
Ultrasound of GI function
Ultrasonographic function examinations are performed to determine motility in the gastrointestinal system. Other methods such as esophageal manometry and scintigraphy are commonly used but are limited due to invasiveness or exposure to radioactive radiation. Transabdominal ultrasonography does not interfere with normal motility and does not give off harmful radiation, thus proving a suitable method for studying gastrointestinal movement patterns.
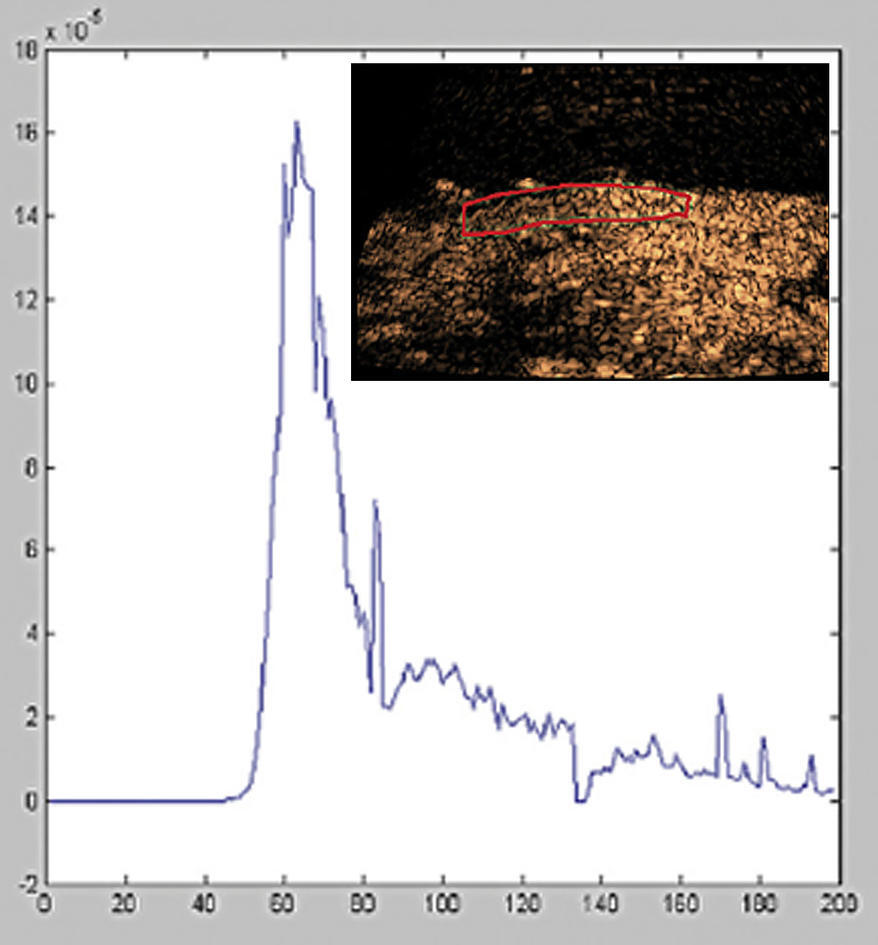
Sonoelastography – Strain Imaging
Sonoelastography is a technique that registers tissue density. The term elastography is used for several related ultrasound methods that measure stiffness in the liver by sending impulses into the liver tissue. Elastography has no known side effects, does not cause pain or discomfort and is experienced as a regular ultrasound examination for patients.
Sound waves conducted in tissues, such as the liver, change speed depending on the density of the tissue. Cancerous and/or damaged tissues often have a higher density than normal, and this can be detected by of elastographic principles. The pulse wave moves faster in rigid tissue than in elastic tissue, and the velocity therefore correlates with the level of stiffness, which in turn correlates with the degree of fibrosis. Based on these measurements, computers can provide an image of an organ and show variations in tissue density throughout the organ. Elastography has become most widespread by detecting fibrosis after inflammation in the liver, thus reducing the need to take tissue samples from the liver.
CEUS – Microbubbles
Contrast-enhanced ultrasound (CEUS) is the application of an ultrasound contrast agent during the ultrasound examination. The ultrasound contrast agents used are based on microbubbles contained in lipid shells. The bubbles contain a gas that reflects sound waves, resulting in a stronger signal from the bubbles. Areas containing the contrast agent will therefore give more signal back to the ultrasound probe and will appear brighter on the image. The bubbles are small and spread in the bloodstream. They will break after some time, the gas will be absorbed into the blood and the contrast agent is eliminated through respiration. The use of contrast ultrasound to characterize liver lesions has become widespread and over 30 other clinical applications are established.
Endosonography Endosonographical methods are minimally invasive, developed for various organ systems accessible through natural or artificial bodily cavities. In endoscopic ultrasonography (EUS), ultrasound transducers are combined with dedicated endoscopes. or by leading miniature probes via the working channel in a conventional endoscope. High-frequency sound waves produce detailed images of the walls and linings of nearby organs such as the liver and the pancreas. EUS allows sampling of fluid and tissue for analysis when combined with fine-needle aspiration. EUS is also very suitable for various interventions, such as draining pseudocysts or abscesses and radiofrequency ablation.
Ultrasound-mediated therapy
Ultrasound-mediated targeted delivery (UMTD) is a delivery modality of therapeutic materials based on ultrasound. By linking therapeutic constituents with ultrasound contrast agents, UMTD enables micro bubbles to, through different mechanisms, open pores in the cell membrane and increase drug efficiency. This method is showing great potential in biomedical applications and BRUSE was the first group ever to treat cancer patients with this new concept.
Gastrointestinal Ultrasound (GIUS) in IBD
Due to changes in treatment regimens and treatment goals for inflammatory bowel diseases, there is an increasing need for close monitoring. Improvements in image quality and resolution on ultrasound scanners have led to a clear view of the wall of the gastrointestinal tract and its separation from surrounding structures. Since GIUS is also a patient-friendly method, it has found its place in the follow-up of IBD patients. To improve the standardization and increase the use of GIUS in the daily follow-up of patients, there is a need for new clinical studies that look at relevant patient populations and compare accepted reference standards. Ongoing longitudinal observational studies examine clinical outcomes in inflammatory bowel diseases and, depending on the result, this could lead to projects where we use GIUS as a tool for clinical decisions.